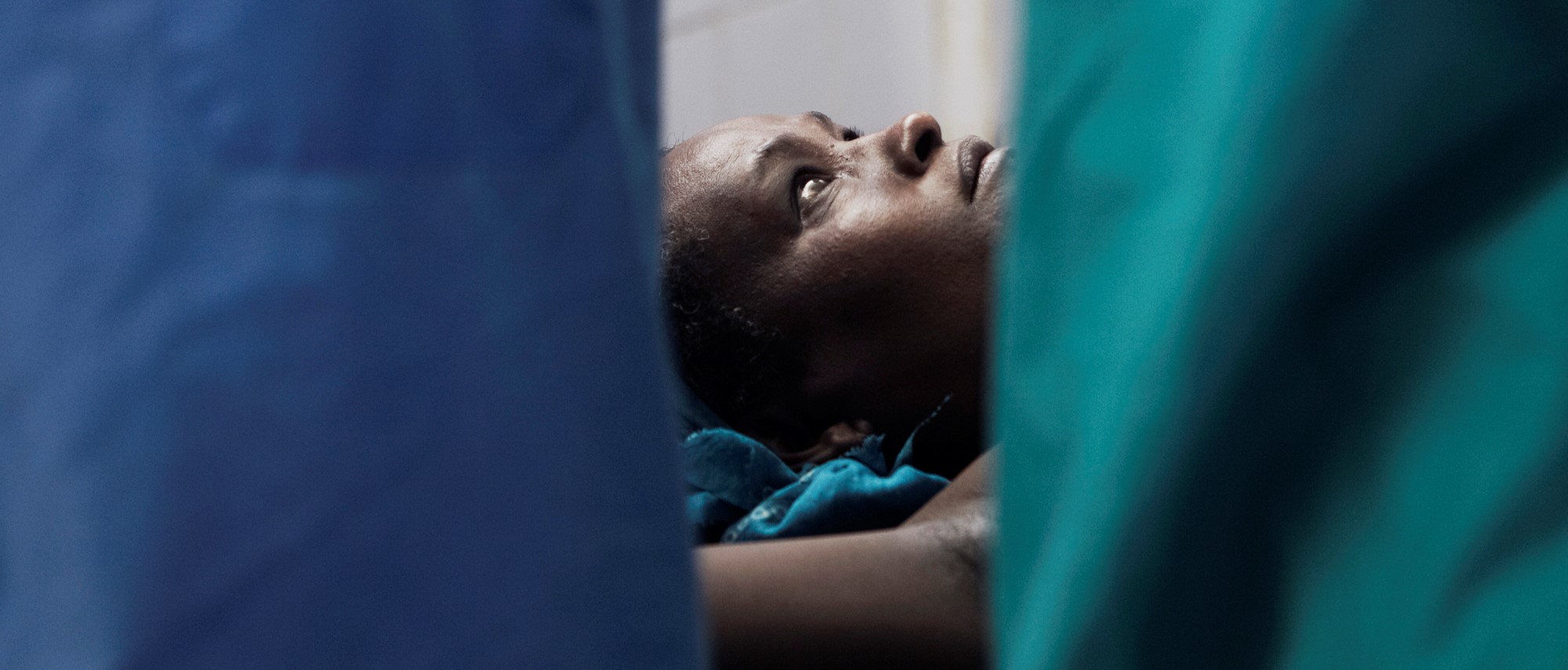
Dead women don’t cry – why women’s health is an inequality matter
As a young doctor in 2004, Henriette Svarre Nielsen travelled to Ethiopia to work as an obstetrician. Four months later, she returned to Denmark with a forever changed view on maternal mortality as a social and global problem. Immediately after, she founded Maternity Foundation. This is her story – as told in our anniversary book in Danish, and now translated in English.
“You fly for 12 hours, and then you drive for 12 hours. And then you are in a completely different world. In 24 hours, you have travelled 100, maybe 200 years back in time. It is here, in Gimbie in Western Ethiopia that I start to grasp the world’s inequality. In the Ethiopian highlands you do not plan your pregnancies. There is no knowledge of or access to family planning, and in the Ethiopia I visit in 2004, it is a gamble with your life to give birth.”
That is also the case for Aryele, a beautiful, pregnant, 16-year-old Ethiopian girl. As I cut open the soft part of her baby’s skull, its yellow brain mass runs out. Her little baby boy is already dead, and the reason I am performing this gruesome procedure on an unborn, dead baby is to save Aryele, who arrived at our hospital after three days of walking with contractions. Her journey started after she had been in labour for two days at home without any progress. After the third day, there is no longer any signs of life in her belly, and when she reaches the hospital in Gimbie where I examine her, I quickly realise that this woman will not be bringing home a living baby.
Aryele is skinny and her body is still not fully developed, most likely due to a life of under- and malnutrition. She got pregnant immediately after she was married off at 15, but the little boy she is carrying did not survive three days of walking in rough terrain and with frequent contractions. He is too big to be delivered naturally, so I perform a craniotomy, which I once saw a description of in an old obstetrics book at home; I cut open the baby’s skull to reduce the head size and enable the baby to come out. I do it to save his mother’s life.
Where am from, craniotomies during labour belong in the past, and babies who are too big for a natural delivery are delivered through a C-section. In Gimbie, C-sections are for the lucky few, and since Aryele’s child did not make it to the hospital alive, it would be extremely dangerous to do a C-section. When cutting her open, you risk releasing toxins that prevent the blood vessels from closing. The woman can go into shock and die of bleeding
Aryele survives. She and her husband bring their dead baby home in a cardboard box.
The land of childhood dreams
It is a coincidence – but then again not really – that I find myself in an operating room in Ethiopia. Because Ethiopia was always there in my life. My mother grew up there, my grandparents were missionaries and had worked with hospitals in Ethiopia for 15 years, and their home in Denmark was full of Ethiopia. The photo of the Ethiopian emperor Haile Selassie and my grandfather hung on their wall and was always the source of good stories. We often watched their photos from Ethiopia, and I had an almost fairytale-like image of the place, but I also knew that it was a country struggling with great poverty and political unrest. All the trips to Ethiopia that my mother always talked about never happened. But I guess I have always known that I would end up working in Africa.
In 2004, I had my first son, Elias. I was a young doctor pursuing my specialty in gynecology and obstetrics, and I was sending one application after the other for PhD-projects on gender inequality within my field, but I never received any funding. That was my first lesson: There is limited interest in women’s reproductive health. You can not get funding. One day I went home to my husband and said, ‘Elias and I are going to Africa’. My husband did not exactly love the idea of being separated from us for four months, so we arranged that they would be with me some of the time in Ethiopia. And so I went.
My mother still knew people in Ethiopia, so through her contacts I arranged to start in the capital Addis Ababa to observe and learn fistula operations and then go and work from a rural hospital in Gimbie. Up until then I had only read about fistula, which occurs during labour when a contraction cuts off the blood supply. If the woman is in labour for several days, the tissue breaks down, and it can cause tears between the vagina and the bladder – and sometimes also the rectum. That means that everything exits through the vagina.
Women with fistula suffer from permanent incontinence. They smell, and on top of their health problems, they are stigmatised. It is a very common consequence of fistula to be socially shunned. Gynecologically speaking, this shouldn’t even happen, but WHO estimates that more than two million women are living with fistula. After my training in in Addis Ababa, I travel to Gimbie to start up a fistula project, where we reach out to women in the area through radio and other channels, encouraging them to come to us and have a fistula operation.
Who will speak up for her?
At first, no one shows up. I start to wonder if the numbers from WHO are wildly overrated. But then slowly, they start coming.
One of my first patients is a 17-year-old girl. At 14, she was raped by the man of the house she worked in, she got pregnant and had a fistula. Her family kicked her out because of the smell from the fistula, but now her mother is bringing her to us at the hospital. We operate on her and make her ’dry’ again. And suddenly I see a completely different young woman in front of me.
But I also see the world’s inequality and injustice in her story: she was raped, she is malnourished and too tiny to give birth, and on top of it all she gets a fistula and is kicked out. What rights does she have? Who will speak up for her? It is heartbreaking, and even though I came to Ethiopia with a clinical interest, this issue of inequality is taking up more and more of my headspace. I start noticing how little women’s health matters, and how they have significantly fewer rights than men. But at least we get to operate all these women. And it feels amazing to accomplish that.
I came to Gimbie to do fistula operations and not to be an obstetrician, but it quickly turns out that, as a young doctor in a hospital where not much is working, I am the one with the most skills when emergencies occur. There is a Filipino doctor at the hospital, but he does not want to get up at night to work, and there I am, capable of doing c-sections and managing post-partum haemorrhage. I quickly end up doing most of the shifts, while Ruth Lawson, a superb British doctor and co-founder of Maternity Worldwide, who I meet out there, covers for me when I need to sleep. In Gimbie, I am the person in charge of emergencies, where in Denmark I would have a whole team to consult with. Here, you just react. New emergencies are constantly happening. But it is actually going quite well, and I remember feeling this high, because I was managing it.
Our memory is short
One of the things that strike me in Gimbie is thatpregnant women do not seem excited to be having a baby. And even those giving birth to a healthy baby, do not seem happy. I was puzzled by that. Where was the joy and their connection with their baby? Was it because they didn´t understand me when I was talking to them? Was it something cultural that I didn´t understand? Today I know that it is a survival mechanism to not get excited too soon, because you can so easily lose your own or your baby´s life.
It starts to increasingly upset me that these women not have access to a safe childbirth. We are not speaking high-tech here. We can fairly easily prevent women and babies from dying in childbirth if we make sure that the woman gives birth at a heath facility and if the health workers helping her know what they are doing. It is mostly common sense and minor practical procedures that save these women.
Almost 90% of these deaths can be prevented but where I am in 2004, only 2% of births happen at a hospital and antenatal checkups are almost non-existent. Here, the cause of death for one in seven women is bleeding – just like women in Denmark used to die of bleeding after birth. It is not that long ago that giving birth was also very dangerous for women in Denmark. But we tend to forget that. Our memory is short.
The contrasts were too great
Up until then I had enjoyed my life in Denmark, but in Ethiopia I slowly start to realise not just the gender-based inequalities but the massive global inequalities, and when I return to Denmark four months later, I do not know how to function at home.
The Ethiopia trip is taking up all my headspace, I not relate to everyday things at home, and all I can think of is how insanely privileged we are, being born in a country like Denmark. When I hear people complaining about tiny, everyday things in Denmark, my thoughts immediately go back to Ethiopia: Back to all the poverty. Back to the fistula hospital and the operation rooms where we would operate on four women at the same time in the big open room with very little sanitation. I realized I needed to find a way to process my experiences. Either I needed to let go and become my old self. Or I needed to do something. I knew I needed to do something. After having seen how bad things were, I had to take responsibility and act. That was the beginning of Maternity Foundation.
A mother’s life
From the very beginning, our focus at Maternity Foundation was the very basic humanitarian perspective: We obviously cannot leave women to die during childbirth. That perspective becomes very concrete once you have a bleeding woman on your table. Then you do whatever is necessary.
But good obstetric care goes way beyond the individual life saved. We know the ripple effects of saving a mother’s life extend to the survival of her child, and her contributions to her community. You need to keep that in mind whether you are in the maternity ward at a Danish or an Ethiopian hospital. And that is why we focus on both the village and the hospital – to make sure that the family knows that the woman needs to come to the clinic or hospital. Make sure they know to secure transport in advance. Make sure that the health workers at the hospital know what to do. That is the key to fight this inequality and make a woman’s life as much worth as a man’s.
Every other minute, a woman dies from complications related to pregnancy and childbirth. is 300,000 women every year, 800 women every day. We are closing our eyes to it. Maybe we would notice it more if every day, two airplanes full of pregnant women crashed. But as of now, not enough people are speaking their case.
Dead women do not cry, and as soon as you are gone, your voice is gone. But global problems of poverty, inequality and over-population are not solved by letting women and babies die. The woman is the center of the family in these communities, and when she dies, the family often shatters to pieces. We know that educations is key to a lower birth rates, but these children who could have been their country’s next doctors, engineers and nurses instead become motherless – and the consequences are catastrophic: lack of education, lack of social security and a high risk of a life with crime or prostitution. It is the beginning of a vicious cycle. So apart from the obvious moral obligation to save these mothers’ lives, it is also of outmost importance for financial stability and political stability.
We have a responsibility
Maternal mortality is a pretty accurate indicator of gender equality I see the inequalities within health, also between men and women. When I started studying medicine, I had this idea that there is no difference between men and women when it comes to health equity. Today, I find it deeply interesting to see how women’s health is perceived globally, and that the main indicator is maternal mortality. We measure women’s health based on how many women die in childbirth. That continues to shock me. It is a grotesque and disproportionate health measurement.
It is under the Ethiopian stars and during the many conversations and experiences I have at that time, that I begin to fathom the consequences of the immense inequality between rich and poor countries, and not least between a well-functioning health system and one that barely exists. To lose a wife or a mother ill not solve any problems. The global community has acknowledged that and included it in the UN Sustainable Development Goals.
Unfortunately, there are many issues preventing this from being achieved: lack of education and financial resources, culture, and traditional gender norms in the communities – as well as religious powers in the Western world, who are against family planning. And because of that, pregnant and birthing mothers are still dying.
Creating access to reproductive health takes a holistic, long term, broad and sustainable approach with a global focus on strengthening women’s financial status and position in and improving health systems.
For me, that yellow brain mass will always be a reminder of this world’s deep inequalities. And of our responsibility to save lives.
- In 2005, after having worked in Ethiopian hospitals for four months, Henriette Svarre Nielsen takes the initiative to start Maternity Foundation, of which she is currently the chair of the board.
- Today, she works as MD and professor in Obstetrics and Gynecology at Hvidovre Hospital in Copenhagen. She is leading a research project focusing on infertility problems in Denmark.
- This year, Maternity Foundation is celebrating our 15th anniversary. This article is an English translation of a chapter in our Danish anniversary book, and we will be releasing more translations throughout the year.
You can buy our anniversary book, Det må ikke koste liv at give liv, (in Danish) here.